Excuses for excess deaths
NHS does not accept claims of Royal College
HART Group
Mar 26, 2023
01:27 PM
The Royal College of Emergency Medicine claims that over 20,000 people died in 2022 after waiting for care for at least 12 hours. They say these deaths resulted from long delays in A&E, where emergency departments are frequently overwhelmed and unable to find patients a hospital bed. The claim is based on modelled data which showed that patients who waited longer for a bed had a higher mortality. No consideration seems to have been given to the fact that patients who needed specialised care such as a bed in a coronary care unit might well have had to wait longer and might well have a higher baseline mortality rate.
The claim does suggest that the Royal College of Emergency Medicine does not trust its members to triage patients effectively to ensure those whose lives are at risk get the care they need. It is possible that the rise in A&E waiting times is not the root cause of the problem, but rather a symptom of an overwhelmed healthcare system. This may be due to an increase in the number of patients with severe conditions or an inability to discharge patients to care homes.
If there really was a rise in deaths due to increased waiting time there would be a rise in excess mortality in hospitals. The data on deaths in hospitals does not reflect that. After the lockdown / covid waves, hospital deaths began rising in mid-2021 and remained at higher levels, albeit with a quieter than usual winter in 2021/2022. Deaths in hospital have been below the 2015-2019 average since mid February 2023 according to ONS.
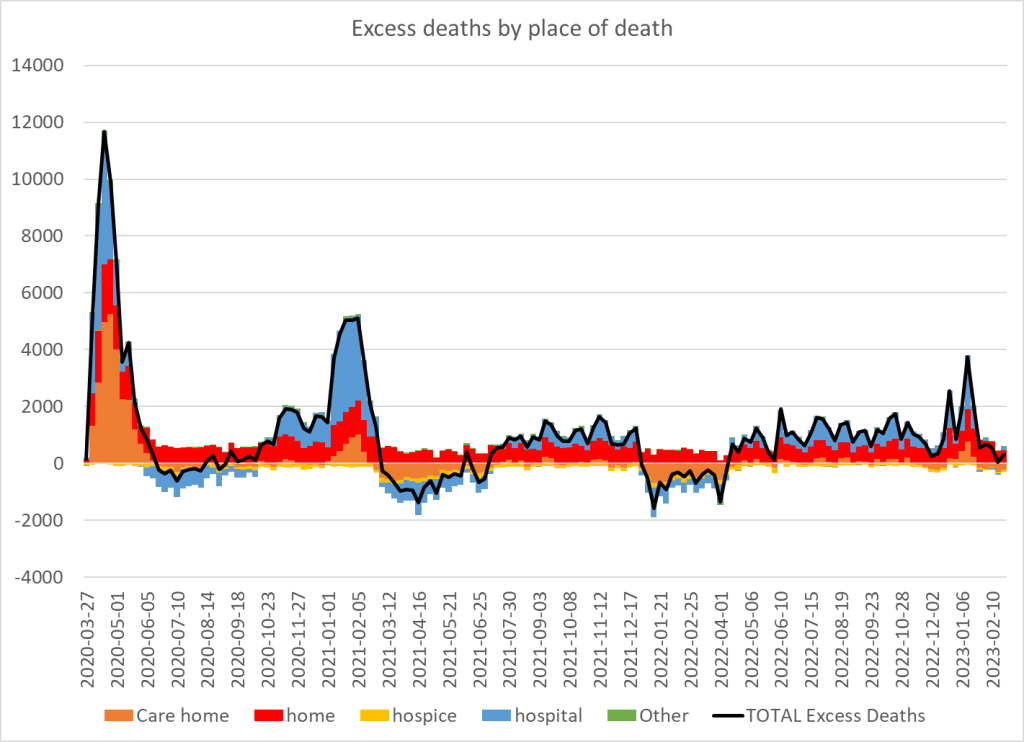
Figure 1: Excess deaths by place of death UKHSA data
NHS England disputed the findings. A spokesperson said “The cause of excess deaths is down to a number of different factors and so attributing deaths to one exact thing, as the figures quoted by the RCEM attempt to do, is very unlikely to give a full or certain picture.”
In reality, although there was an excess in hospital deaths in 2022 the numbers dying in excess was always higher for those dying at home than in hospital.
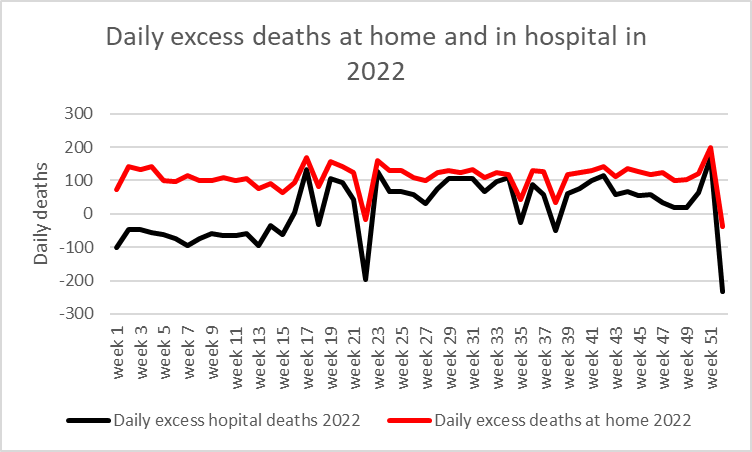
Figure 2: Daily excess deaths at home and in hospital ONS data compared to 2015-2019 baseline
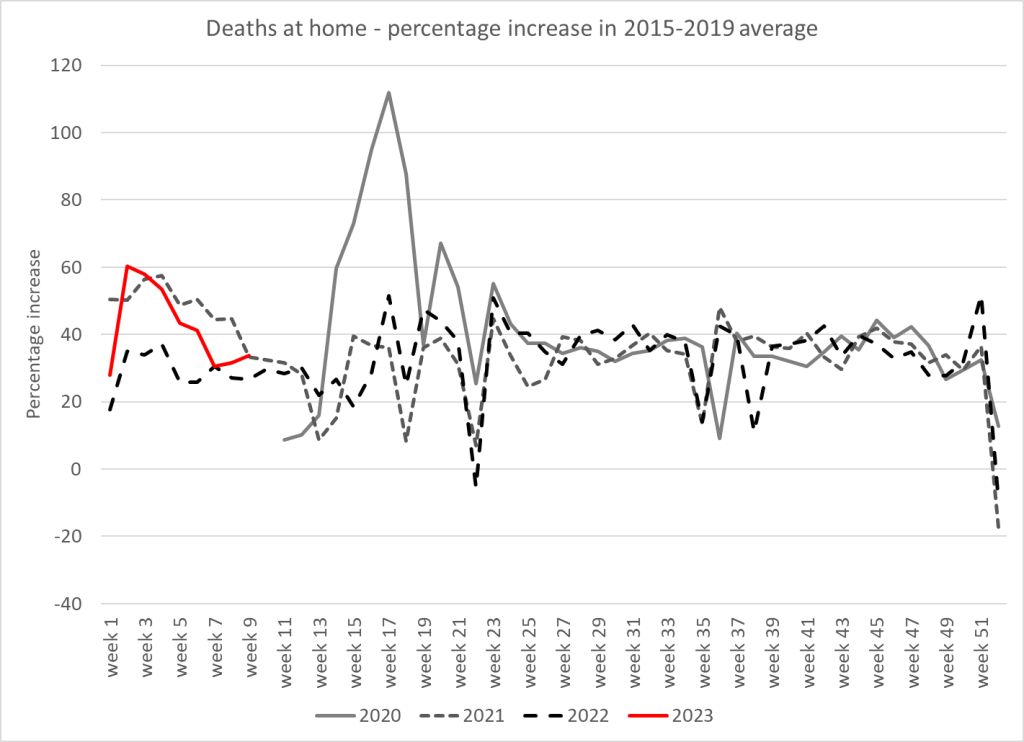
Figure 3: Deaths at home as a percentage increase above 2015-2019 levels since March 2020
The number of deaths that occur at home continue at around 100 more every day than the 2015-2019 average. For three years deaths at home have been between 20-60% above 2015-2019 levels with a further spike in the first lockdown. Yes, some may be patients who would have died in hospices or in hospital in the past. However, a proportion will be sudden deaths. During lockdowns these may have included patients who did not ask for help or were turned away, as highlighted by pathologists in Oxford. There may have been patients who could have had their lives extended in hospitals but because of visitor restrictions chose not to be admitted and died at home. Why have we now still got an excess of such deaths?
This article was originally published by HART Group and is republished here with permission
